Bedsore (Pressure Ulcer) Prevention & Treatments
Medically reviewed by Dr. Xavier Chong Shin Thong , MD
Founder of GP House Call , Ex- Medical Officer in Sultanah Fatimah Specialist Hospital, Muar
What Are Bedsores and Why They Matter
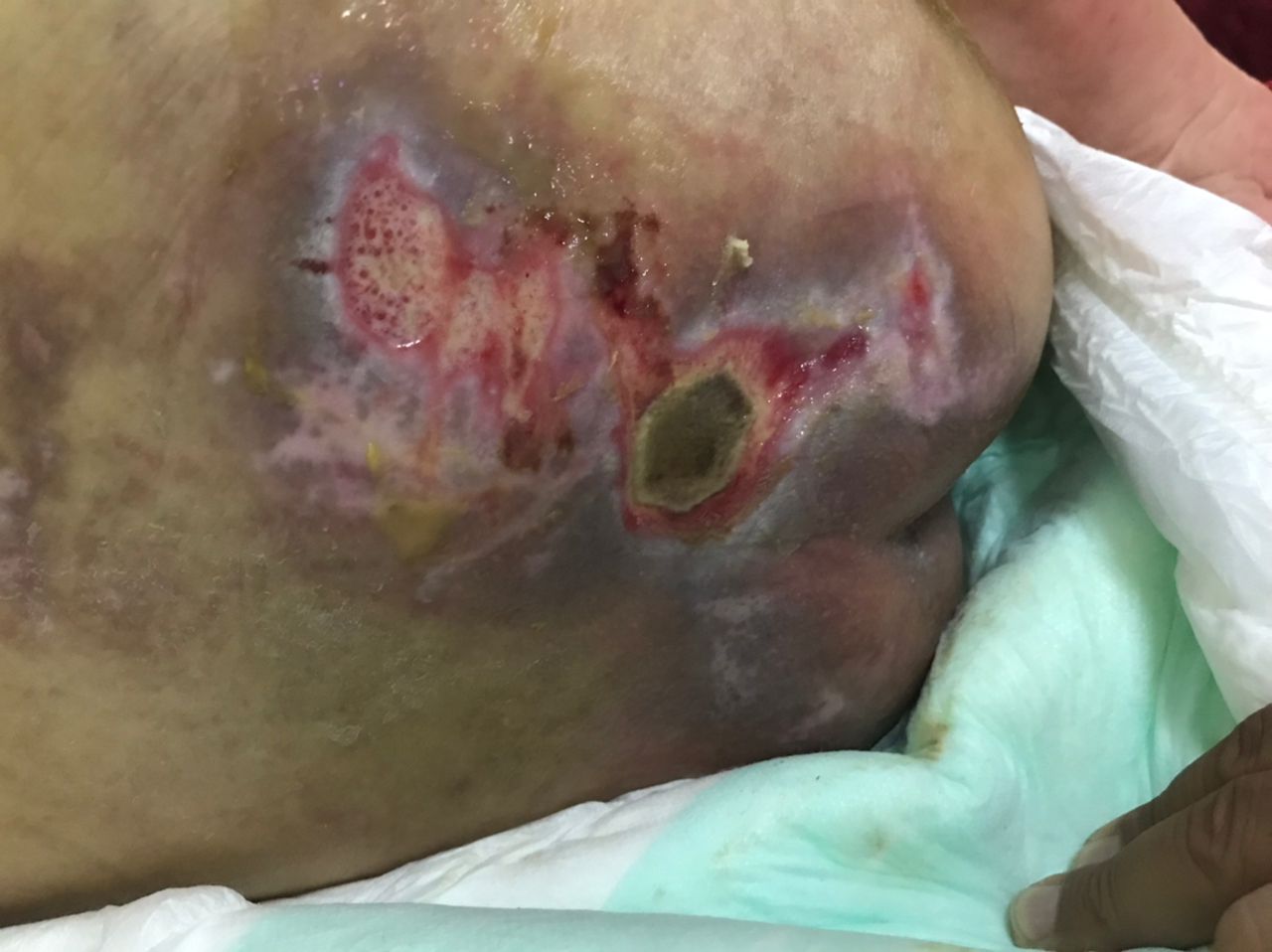
Bedsores, also known as pressure ulcers, are skin and tissue injuries caused by prolonged pressure that restricts blood flow to certain areas.
They are especially common among bedridden patients, wheelchair users, or people with limited mobility. Without proper care, these wounds can progress quickly and lead to serious complications such as infection or sepsis.

1. Relieve Pressure on the Affected Area
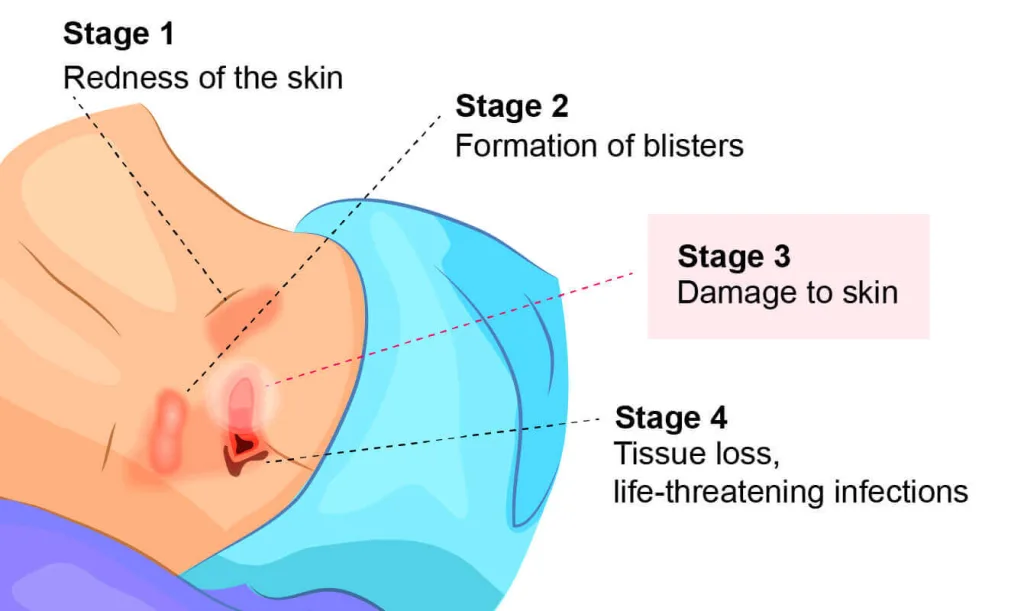
First and foremost, relieving pressure is the most important step in both prevention and treatment. Bedsores typically develop on bony areas — such as the hips, heels, or tailbone — due to continuous pressure.
If someone is bedridden, reposition them at least every two hours to avoid prolonged stress on one spot.
💡 Tip: A home visit nurse can create and maintain a safe repositioning schedule for individuals requiring long-term care.
2. Keep the Wound Clean
Cleanliness plays a crucial role in preventing infection and promoting healing. Always clean the bedsore using sterile dressing techniques and approved antiseptic solutions, under the supervision of a qualified house call doctor.
According to the Mayo Clinic, maintaining proper wound hygiene and moisture balance is key to recovery.
3. Healing Agents and Medications
Choosing the right dressing can significantly speed up healing.
Commonly used dressings include:
Hydrocolloid (retains moisture)
Foam (cushions and protects)
Alginate (absorbs excess fluid)
If an infection is suspected, a doctor may prescribe oral or intravenous antibiotics to control bacterial growth.
4. Support Healing with Proper Nutrition
Nutrition is equally important in recovery. A balanced diet rich in:
Protein – supports tissue repair
Vitamin C – aids collagen production
Zinc – boosts wound healing
Research published in PubMed confirms that malnutrition can delay wound recovery in individuals confined to bed.
5. Advanced Medical Procedures
For stubborn or severe pressure ulcers, advanced treatments can make a difference:
Wound debridement – removes dead tissue, allowing healthy skin to regenerate.
Regenerative therapies – such as Platelet-Rich Plasma (PRP) injections to speed up recovery.
These procedures can be safely done at home by trained medical professionals.
6. Use Pressure-Relieving Devices
Finally, prevention tools such as pressure-relieving mattresses and cushions help reduce recurrence.
For example, a ripple mattress system alternates air pressure between cells, mimicking natural movements during sleep and lowering stress on the same area.
Why Prevention Is Always Better
Preventing bedsores is far easier — and less painful — than treating them.
With regular repositioning, skin checks, proper nutrition, and supportive devices, individuals with reduced mobility can maintain healthier skin and avoid the discomfort of pressure ulcers.
For more clinical details, visit the Cleveland Clinic’s Bedsore Guide.
Frequently Asked Questions (FAQ)
Q1: Who is most at risk for bedsores?
Anyone who is immobile for long periods — including those recovering from surgery, wheelchair users, and people requiring long-term bed rest — has a higher risk.
Q2: Can bedsores heal completely at home?
Yes, if detected early and treated properly under medical guidance. Severe cases may still require hospital-based care.
Q3: How long does a bedsore take to heal?
Mild sores may heal in 1–3 weeks with proper care. Advanced sores can take months and require specialised treatment.
Q4: Are pressure ulcers painful?
Yes. They can cause significant discomfort, especially if infected or deep. Pain relief should be part of the treatment plan.
Q5: How often should repositioning be done?
Ideally, every two hours for bedridden individuals and every 15–30 minutes for wheelchair users.
Conclusion
Bedsores are preventable with consistent attention and proactive measures.
Whether you are caring for a loved one at home or recovering from an illness, a doctor house call can provide safe, effective, and personalised care — right at your doorstep.
Taking steps today not only prevents complications but also supports faster healing and a better quality of life.
Related GP House Call Services